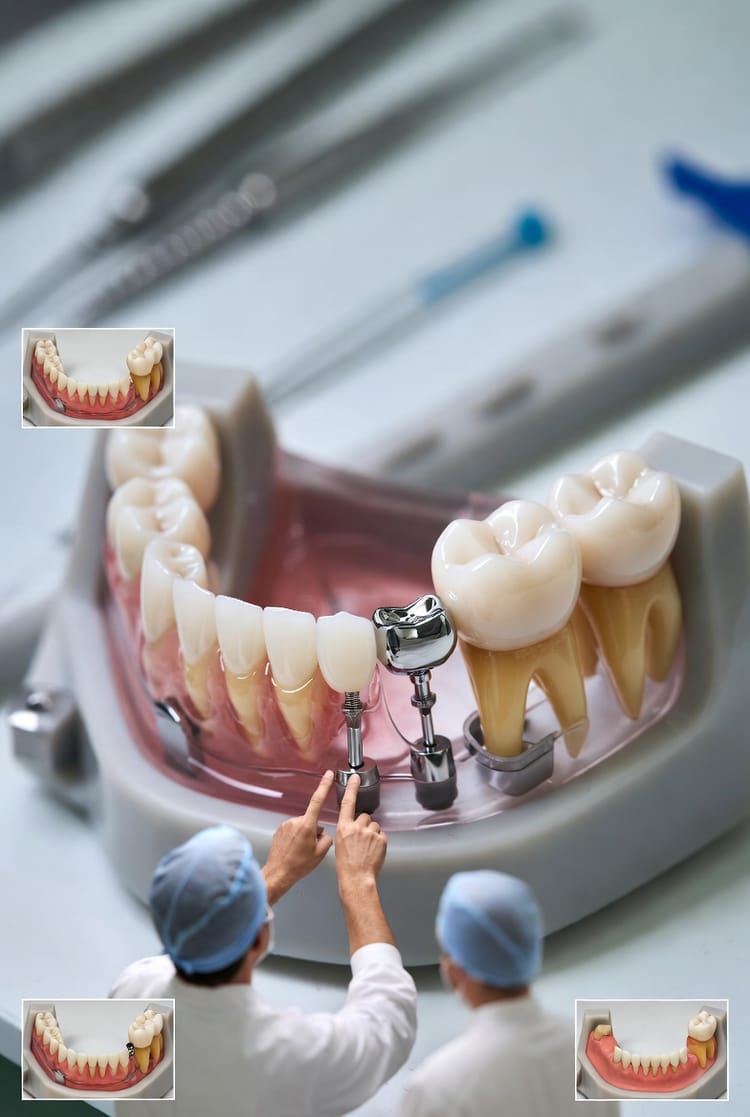
The Dry Socket Prevention: What Happens After Tooth Extraction and How to Avoid This Painful Condition
Undergoing a tooth extraction can be a straightforward procedure, but what happens afterward is crucial for your comfort and recovery. As a leading voice in dental health, we're here to guide you through the process with confidence. Dry socket, medically known as alveolar osteitis, is a common yet preventable complication that affects about 2-5% of patients after tooth extractions, particularly wisdom teeth removals. Rest assured, with proper knowledge and aftercare, you can minimize risks and promote smooth healing. In this comprehensive guide, we'll explore what occurs post-extraction, define dry socket, highlight risk factors, describe symptoms, and provide detailed aftercare tips. By following these steps, you'll be on your way to a pain-free recovery.
Avoid Painful Dry Socket – Get Your Aftercare Instructions Today
Understanding the Tooth Extraction Process
Tooth extraction involves removing a tooth from its socket in the jawbone, often due to decay, infection, crowding, or preparation for orthodontics. The procedure itself is typically quick and performed under local anesthesia, sedation, or general anesthesia depending on complexity. Immediately after, your body begins the natural healing process.
Once the tooth is removed, a blood clot forms in the empty socket. This clot acts as a protective barrier, shielding the underlying bone and nerves while new tissue grows. Over the next few days to weeks, granulation tissue fills the socket, followed by bone regeneration. Full healing can take 3-6 months, but the initial phase is most critical.
It's normal to experience some bleeding, swelling, and discomfort in the first 24-48 hours. However, complications like dry socket can arise if this clot is dislodged or fails to form properly. Don't worry – armed with the right information, you can avoid this.
What Is Dry Socket?
Dry socket occurs when the protective blood clot that forms in the extraction site is lost prematurely, exposing the bone and nerves to air, food, and fluids. This exposure leads to intense pain and delayed healing. Unlike typical post-extraction discomfort, which subsides within a few days, dry socket pain often intensifies 2-5 days after the procedure.
The condition isn't an infection but an inflammatory response. Without the clot, the socket becomes "dry," hence the name. It's more common after lower jaw extractions, especially molars, due to denser bone and gravity's role in clot stability.
Rest easy knowing that dry socket is treatable. A dentist can clean the site, apply medicated dressings (like those containing eugenol for pain relief), and prescribe antibiotics if needed. Early intervention prevents further complications, such as prolonged healing or secondary infections.
Risk Factors for Developing Dry Socket
Certain factors increase your likelihood of experiencing dry socket. By identifying and addressing these, you can take proactive steps to protect your recovery.
- Smoking and Tobacco Use: Nicotine constricts blood vessels, impairing clot formation. Chemicals in tobacco also irritate the socket. Smokers are up to 4 times more likely to develop dry socket. If you smoke, quitting at least 24 hours before and after extraction is essential.
- Using Straws or Sucking Actions: The suction from straws, smoking, or even vigorous rinsing can dislodge the clot. Avoid these for at least 72 hours post-procedure.
- Poor Oral Hygiene: Inadequate cleaning allows bacteria to thrive, increasing inflammation and clot breakdown. However, gentle hygiene is key – we'll cover how later.
- Previous History: If you've had dry socket before, you're at higher risk. Inform your dentist for preventive measures like sutures or special dressings.
- Oral Contraceptives: Higher estrogen levels in birth control pills can affect clotting, slightly elevating risk for women.
- Traumatic Extractions: Complicated surgeries, like impacted wisdom teeth, involve more bone manipulation, heightening chances.
- Age and Health Conditions: Those over 30 or with conditions like diabetes may heal slower, indirectly boosting risk.
By minimizing these risks, such as staying hydrated without straws and maintaining a smoke-free environment, you'll support your body's natural defenses.
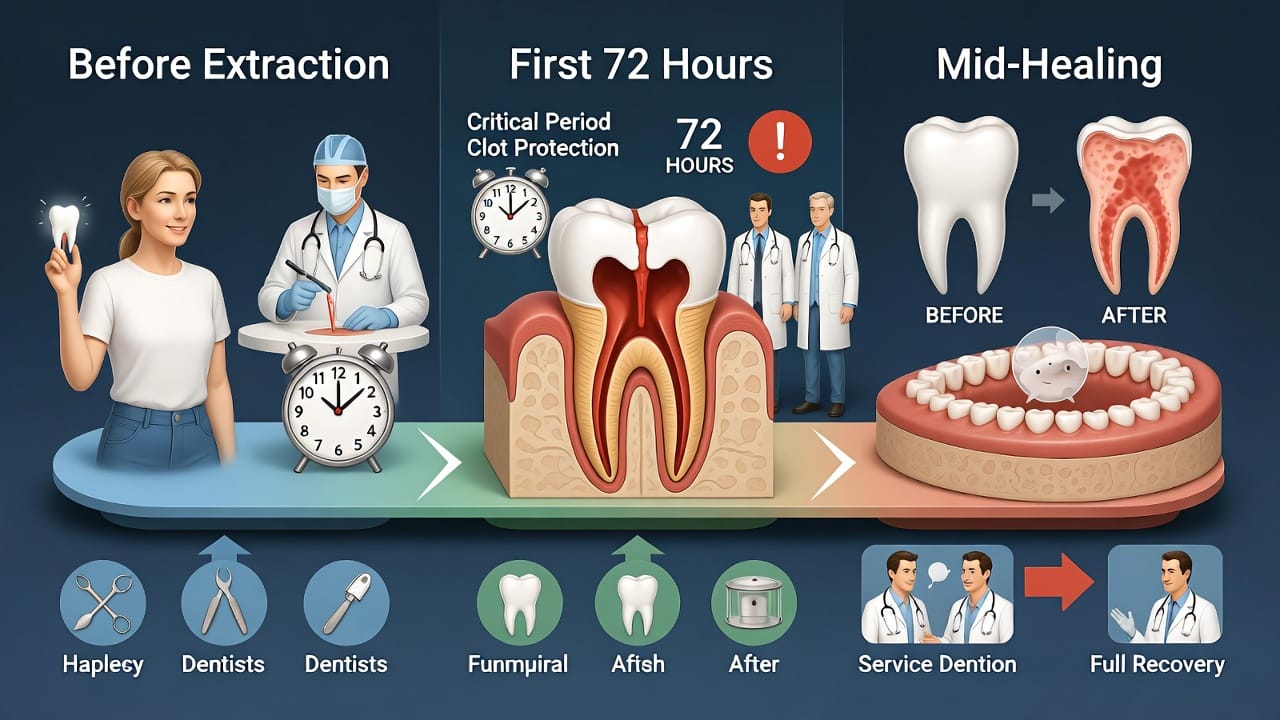
Recognizing Symptoms of Dry Socket
Early detection of dry socket symptoms allows for prompt treatment, reducing discomfort. Unlike standard post-extraction pain, which is manageable with over-the-counter meds, dry socket symptoms are distinct and severe.
- Intense, Throbbing Pain: Starting 2-4 days after extraction, pain radiates to the ear, eye, or temple on the same side. It feels deep and unrelenting, often worsening at night.
- Bad Breath or Foul Taste: Exposed bone allows debris accumulation, leading to halitosis or a persistent bad taste.
- Visible Bone in Socket: Looking in a mirror, you might see empty socket with whitish bone instead of a dark clot.
- Swelling and Lymph Node Tenderness: Mild swelling may persist or worsen, with tender neck nodes.
- No Improvement with Painkillers: If standard analgesics like ibuprofen don't help, it could indicate dry socket.
If you notice these, contact your dentist immediately. Most cases resolve within a week of treatment, and ignoring them can lead to prolonged issues. Remember, it's not a sign of poor procedure but often tied to aftercare lapses.
Essential Post-Extraction Aftercare Guidelines
Proper aftercare is your best defense against dry socket and other complications. Follow these steps diligently for optimal healing. Your dentist will provide personalized instructions, but here's a general, authoritative overview.
Immediate Aftercare (First 24 Hours)
- Control Bleeding: Bite on gauze for 30-45 minutes. If bleeding persists, use a moist tea bag – tannins help clotting.
- Manage Pain and Swelling: Take prescribed pain relievers. Apply ice packs externally for 15 minutes on/off to reduce swelling.
- Rest: Avoid strenuous activity. Elevate your head while sleeping to minimize swelling.
Oral Hygiene Practices
- Gentle Rinsing: After 24 hours, rinse with warm saltwater (1/2 tsp salt in 8 oz water) 4-5 times daily to keep the area clean without dislodging the clot.
- Brushing: Brush gently around the site, avoiding direct contact for the first few days.
- Avoid Irritants: Steer clear of spicy, acidic, or hot foods that could aggravate the socket.
Dietary Recommendations
- Soft Foods: Stick to yogurt, applesauce, mashed potatoes, and smoothies (no straws!) for the first week.
- Hydration: Drink plenty of water, but sip slowly.
- Nutrient-Rich Choices: Incorporate vitamin C-rich foods like oranges (juiced, not chewed) to boost healing.
Long-Term Healing Tips
- Follow-Up Appointments: Attend all scheduled check-ups to monitor progress.
- Monitor for Complications: Watch for excessive bleeding, fever, or pus, which could signal infection.
- Lifestyle Adjustments: If you're a smoker, use this as motivation to quit – resources like nicotine patches can help.
By adhering to these, you'll promote clot stability and tissue regeneration, ensuring a complication-free recovery.

Preventing Complications Beyond Dry Socket
While focusing on dry socket prevention, it's wise to address broader complications. Excessive bleeding, infection, or nerve damage are rare but possible. Maintain open communication with your dental team.
For instance, if you have underlying conditions like osteoporosis or are on blood thinners, discuss adjustments pre-procedure. Preventive antibiotics may be prescribed for high-risk patients.
Healing varies by individual – factors like age, nutrition, and stress play roles. A balanced diet, adequate sleep, and stress management enhance recovery. If pain persists beyond a week, seek evaluation to rule out issues like bone fragments.
When to Seek Professional Help
Don't hesitate to call your dentist if symptoms arise. Early intervention is key. For example, if pain spikes suddenly, it might indicate dry socket needing a dressing change.
In emergencies, such as uncontrolled bleeding or signs of allergic reaction to meds, head to the ER. Otherwise, your oral surgeon or dentist is equipped to handle post-extraction concerns.
Embracing a Healthy Recovery
Tooth extraction is a step toward better oral health, whether relieving pain or preparing for implants. By understanding dry socket and committing to aftercare, you'll navigate recovery with ease.
Stop Dry Socket Before It Starts – Call Our Dental Team Today