Rewiring the Brain: Understanding the Science of Addiction and Pathways to Recovery

Addiction is often misunderstood as a moral failing or a simple lack of willpower. However, modern neuroscience reveals it as a complex brain disorder, rooted in biological changes that can be addressed and reversed. This article explores the neurological basis of addiction, demystifying concepts like dopamine dysregulation and neural pathways, while highlighting evidence-based pathways to recovery. By understanding how the brain adapts and heals, we can foster empathy, reduce stigma, and empower those affected to seek help. Recovery isn't just possible—it's a scientifically supported process of rewiring the brain for a healthier future.
Take the First Step Toward Rewiring – Call for Confidential Help
The Neurological Roots of Addiction
At its core, addiction hijacks the brain's natural reward system. Our brains are designed to reinforce behaviors essential for survival, such as eating or socializing, through the release of neurotransmitters like dopamine. In addiction, substances or behaviors trigger an exaggerated dopamine response, creating a cycle that's hard to break.
Dopamine Dysregulation: The Pleasure Hijacker
Dopamine, often called the "feel-good" chemical, plays a pivotal role in motivation and reward. In a healthy brain, it surges in response to positive experiences, encouraging repetition. However, addictive substances—such as opioids, alcohol, or stimulants—flood the brain with dopamine levels far beyond natural highs. Over time, this leads to dopamine dysregulation, where the brain reduces its natural production or sensitivity to maintain balance.
Imagine your brain's reward center as a volume knob. Normal pleasures turn it up moderately, but addiction cranks it to maximum, drowning out everyday joys. As tolerance builds, individuals need more of the substance to achieve the same effect, escalating use. This isn't weakness; it's a neurochemical adaptation. Studies from institutions like the National Institute on Drug Abuse (NIDA) show that chronic exposure alters dopamine receptors, particularly in the nucleus accumbens, a key area in the brain's reward circuitry.
The good news? The brain's plasticity—its ability to change—means this dysregulation isn't permanent. With abstinence and treatment, dopamine systems can recalibrate, restoring balance over time.
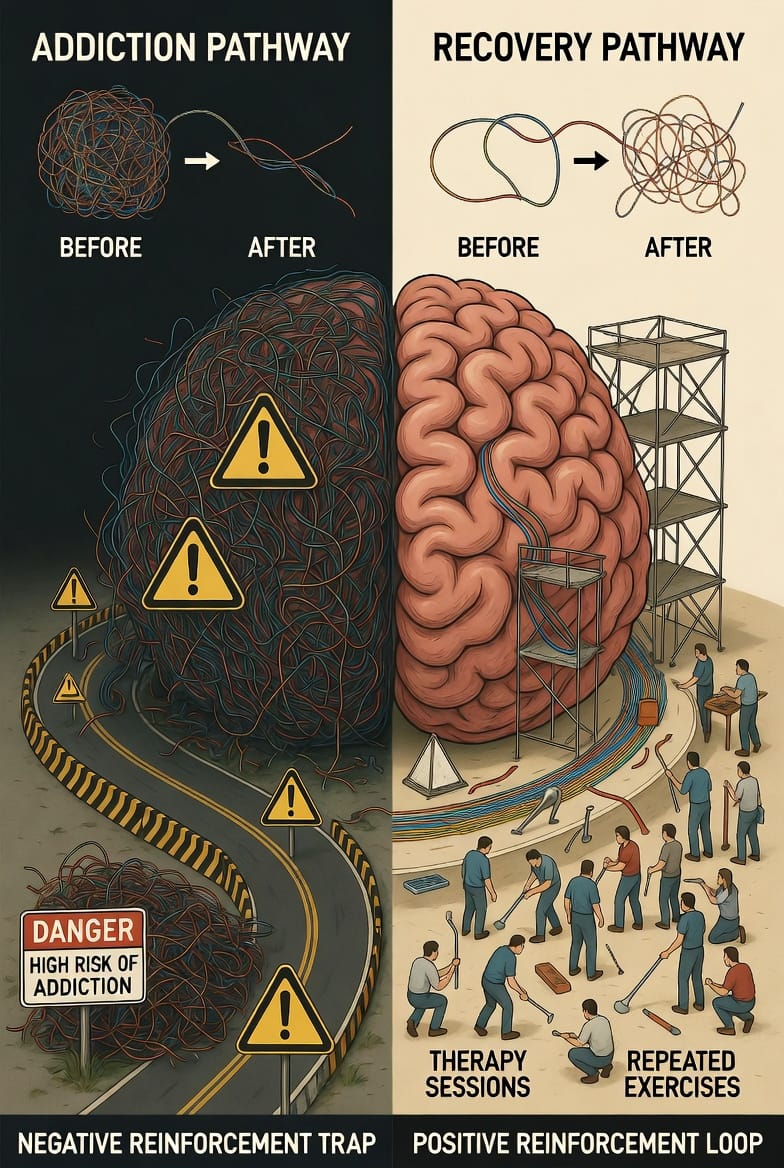
Neural Pathways: The Highways of Habit
Neural pathways are like well-trodden paths in a forest: the more you use them, the stronger and more automatic they become. In addiction, repeated substance use strengthens pathways linking cues (like stress or environments) to the reward of use. This is neuroplasticity at work, but in a maladaptive way.
For instance, the prefrontal cortex, responsible for decision-making and impulse control, weakens under addiction's influence. Meanwhile, the amygdala, which processes emotions, becomes hyperactive, amplifying cravings during triggers. This imbalance explains why logical knowledge of risks doesn't always prevent relapse— the brain's wiring overrides rational thought.
De-stigmatizing this: Addiction isn't a choice but a learned response etched into brain circuitry. Just as we learn to ride a bike through repetition, addiction forms through reinforced behaviors. Fortunately, the same principle applies to recovery: New, healthy pathways can be built to overwrite the old ones.
Pathways to Recovery: Harnessing Brain Plasticity
The brain's remarkable ability to rewire itself offers profound hope. Neuroplasticity allows for healing, even after years of addiction. Evidence-based treatments leverage this by promoting new connections, while time aids natural repair.
Evidence-Based Treatments: Tools for Rewiring
Recovery involves targeted interventions that address both the biological and psychological aspects of addiction.
- Cognitive Behavioral Therapy (CBT): This approach helps reframe thoughts and behaviors, weakening addiction pathways while strengthening coping mechanisms. By practicing alternative responses to triggers, patients literally build new neural routes.
- Medication-Assisted Treatment (MAT): Drugs like buprenorphine for opioids or naltrexone for alcohol normalize dopamine levels, reducing cravings and supporting brain stabilization.
- Mindfulness and Neurofeedback: Techniques like meditation enhance prefrontal cortex function, improving self-regulation. Neurofeedback trains the brain to produce healthier patterns, accelerating rewiring.
These methods are backed by neuroimaging studies showing structural changes: Reduced amygdala activity and restored prefrontal connectivity after consistent treatment.
The Role of Time in Brain Healing
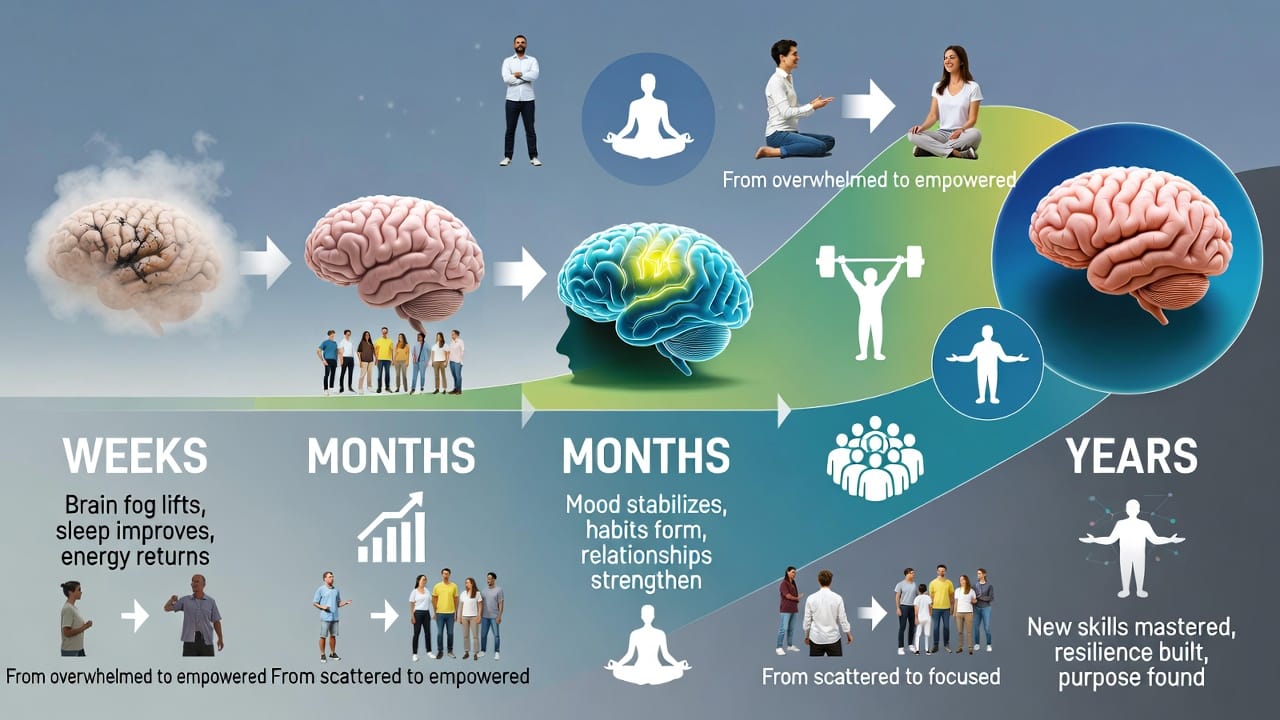
Healing doesn't happen overnight, but milestones mark progress. Early recovery focuses on detoxification and stabilization, while long-term efforts solidify new habits.
In the first weeks, withdrawal symptoms peak as the brain readjusts dopamine levels. Sleep, nutrition, and support mitigate this. By months 1-3, cognitive functions improve, with better focus and reduced impulsivity. Over years, sustained abstinence leads to full pathway remodeling, where healthy behaviors become automatic.
Factors like age, addiction duration, and co-occurring disorders influence timelines, but consistency is key. Research indicates that after 5 years of recovery, relapse risk drops significantly, reflecting deep neural changes.
Building New, Healthy Connections
To foster recovery, it's essential to actively cultivate positive neural pathways. This involves repetition, much like training a muscle.
Therapeutic Repetition: The Key to Rewiring
Therapy isn't just talk—it's practice. Each session reinforces adaptive thinking, gradually diminishing the pull of old habits. For example, exposure therapy confronts triggers in a safe environment, desensitizing the amygdala and empowering the prefrontal cortex.
Group support, like in 12-step programs, builds social connections, activating reward centers healthily. Exercise releases endorphins, mimicking dopamine boosts without substances.
Lifestyle Integration for Lasting Change
Holistic approaches amplify neuroplasticity:
- Nutrition and Exercise: Omega-3s and physical activity promote neurogenesis (new neuron growth) in the hippocampus, aiding memory and mood.
- Sleep Hygiene: Quality rest consolidates learning, helping embed new pathways.
- Stress Management: Chronic stress hinders recovery; techniques like yoga reduce cortisol, protecting brain repair.
By integrating these, individuals not only heal but thrive, forming resilient connections against future challenges.
Navigating Challenges and Preventing Relapse
Recovery isn't linear; setbacks can occur, but they're opportunities for growth. Relapse often stems from unaddressed triggers or incomplete rewiring, not failure.
Neuroscientifically, a slip reactivates old pathways temporarily, but quick intervention prevents full regression. Strategies include contingency management, rewarding sobriety to reinforce positive circuits.
Maintaining hope: Each day without use strengthens recovery pathways, making them the default. Support networks provide external reinforcement during vulnerable periods.
The Broader Impact: De-Stigmatizing Addiction
Viewing addiction through a neuroscience lens shifts the narrative from blame to biology. It encourages policy changes, like increased access to MAT, and personal compassion. Remember, the brain that adapted to addiction can adapt to health— with the right tools and time.
In conclusion, rewiring the brain from addiction is a testament to human resilience. By understanding dopamine dysregulation, neural pathways, and the power of evidence-based recovery, we illuminate a path forward. Recovery is a journey of healing, inside and out.
Start Your Recovery Conversation Now – Call Our Experts


