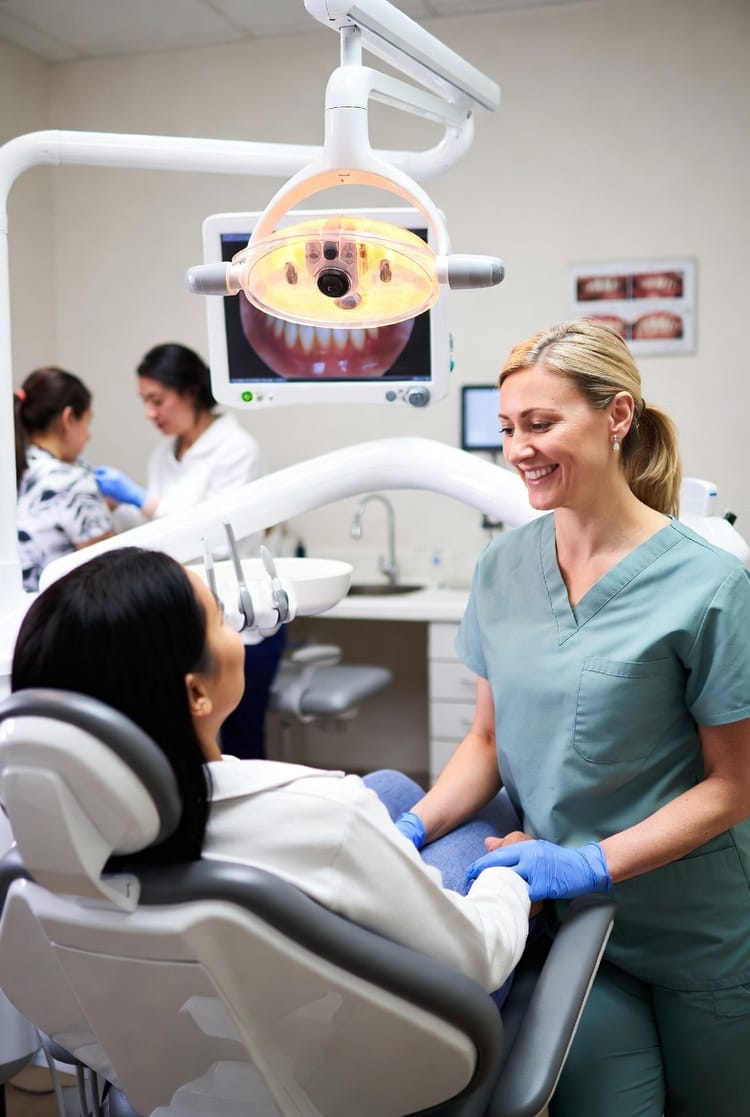
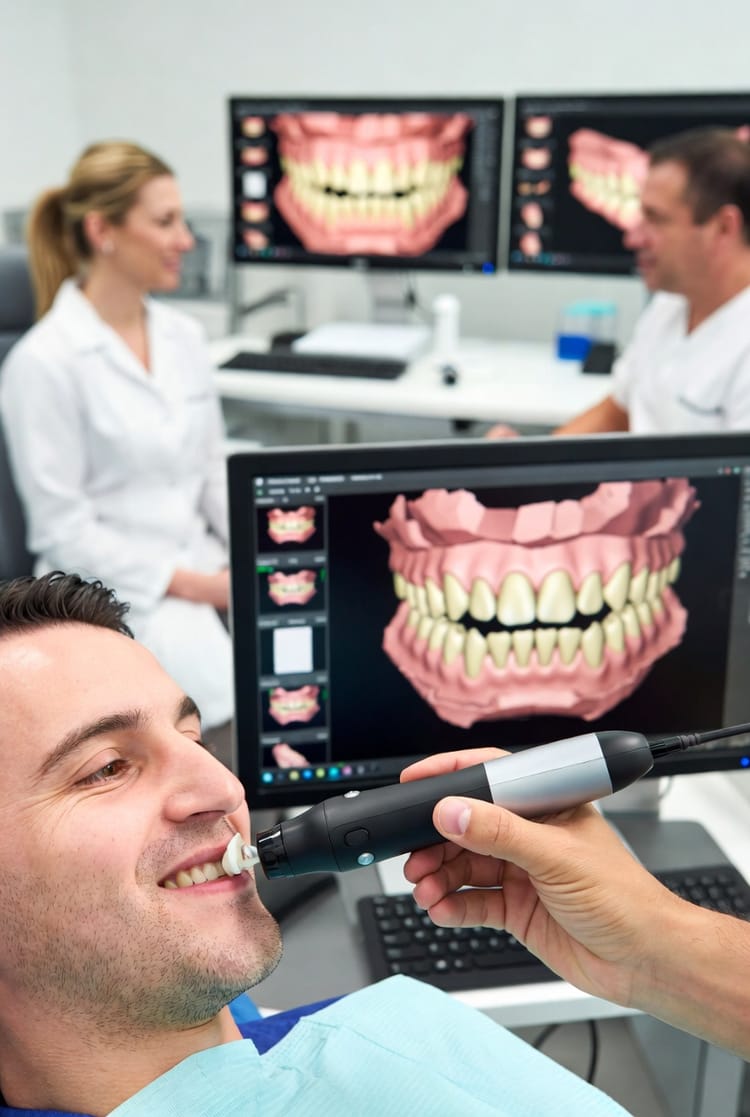
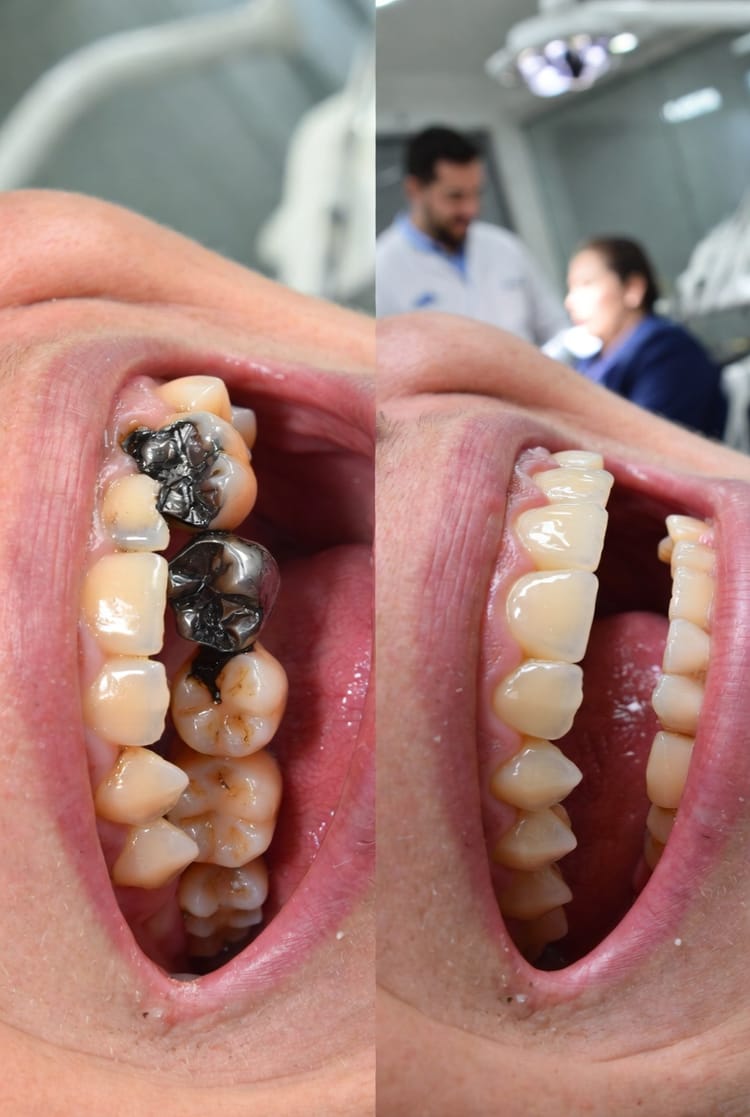
The Mouth-Body Connection in Action: How Periodontal Health Influences Systemic Inflammation
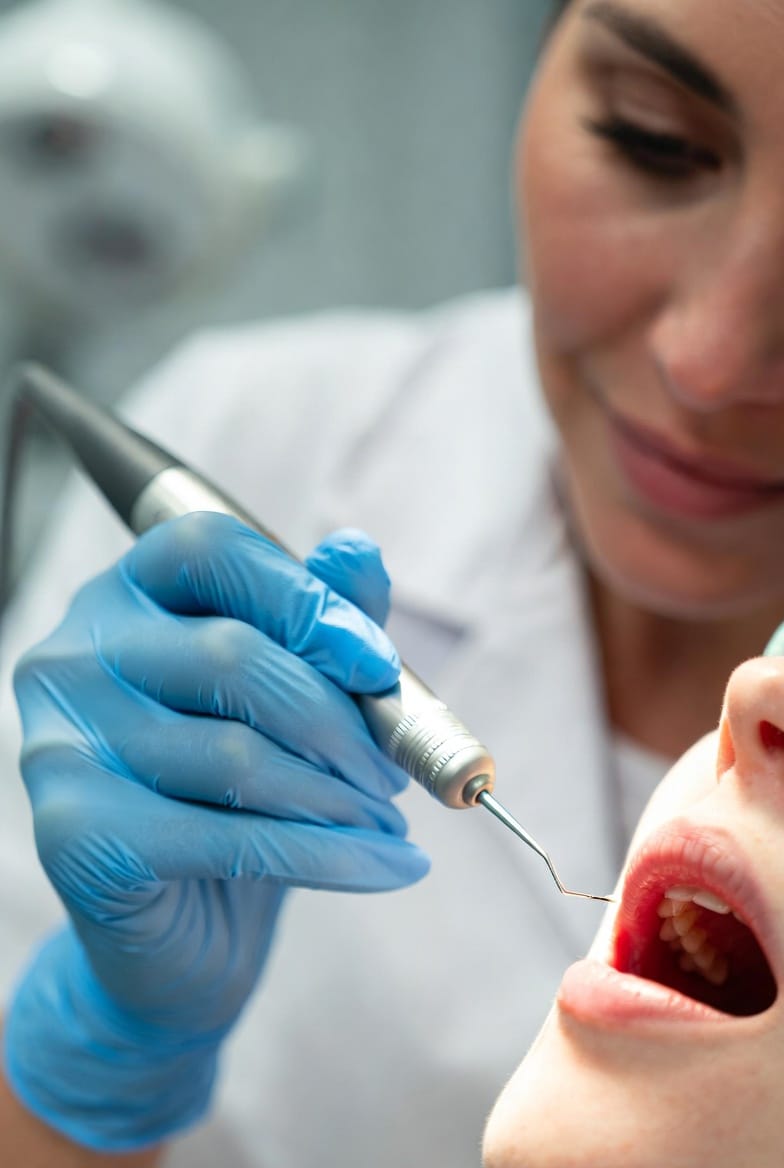
In today's fast-paced world, we often compartmentalize our health—treating our mouths as separate from the rest of our bodies. But emerging science tells a different story. Periodontal health, the foundation of strong gums and teeth, plays a pivotal role in managing systemic inflammation, that underlying fire that can fuel chronic conditions across the body. This article dives deep into the intricate links between gum disease and overall wellness, showing how prioritizing your oral care can safeguard your heart, stabilize blood sugar, and enhance your quality of life. As a reassuring guide, we'll explore evidence-based insights and practical steps, framing preventive dental cleanings not as a mere chore, but as an essential pillar of holistic health.
Schedule Your Preventive Cleaning Today – Protect Your Whole Body
Understanding Periodontal Health: The Gateway to Wellness
At its core, periodontal health refers to the well-being of the tissues surrounding and supporting your teeth—your gums, ligaments, and bone. When these areas are healthy, they form a robust barrier against bacteria. However, poor oral hygiene, stress, or genetic factors can lead to gum disease, also known as periodontitis. This condition starts subtly with gingivitis—inflammation and bleeding gums—but can progress to more severe forms if unchecked.
What makes this relevant beyond your smile? The mouth is a bustling ecosystem teeming with billions of bacteria. In a healthy state, these microbes coexist peacefully. But when plaque builds up and hardens into tartar, it irritates the gums, triggering an immune response. This local inflammation isn't isolated; it has far-reaching effects. Research from institutions like the American Academy of Periodontology highlights how untreated gum disease can contribute to elevated levels of systemic inflammation, where inflammatory markers spill over into the bloodstream, affecting distant organs.
Imagine your gums as the first line of defense in a complex bodily network. When they're compromised, it's like opening a door for chronic issues. But here's the good news: with regular preventive cleanings, you can maintain this barrier, reducing risks and promoting vitality. These sessions, typically every six months, involve professional removal of plaque and tartar, polishing, and personalized advice—turning routine visits into proactive wellness investments.
The Science Behind Gum Disease and Systemic Inflammation
To grasp the mouth-body connection, let's break down the mechanisms at play. Gum disease begins with bacterial overgrowth in dental plaque. Pathogens like Porphyromonas gingivalis invade gum tissues, prompting the release of pro-inflammatory cytokines—chemical messengers that rally the immune system. While this response is protective locally, chronic activation leads to persistent inflammation.
Studies, including those published in the Journal of Clinical Periodontology, demonstrate how these cytokines, such as interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-α), enter the circulation. Once in the bloodstream, they amplify systemic inflammation, a state linked to numerous health challenges. For instance, elevated inflammation can damage blood vessel linings, promoting plaque buildup in arteries—a key factor in cardiovascular disease.
Consider the numbers: People with periodontitis are up to 1.5 times more likely to experience heart attacks or strokes, according to meta-analyses in Circulation journal. This isn't coincidence; it's biology. The inflammatory cascade from infected gums exacerbates endothelial dysfunction, where blood vessels lose flexibility, increasing hypertension risks. Moreover, bacteria from the mouth can travel to the heart, potentially contributing to endocarditis or atherosclerosis.
Shifting to diabetes management, the link is bidirectional. High blood sugar impairs gum healing, making diabetics more susceptible to periodontitis. In turn, gum inflammation worsens insulin resistance, creating a vicious cycle. Research from the American Diabetes Association shows that treating gum disease can lower HbA1c levels by 0.4%—comparable to adding a second diabetes medication. By addressing periodontal issues, you're not just saving teeth; you're stabilizing metabolic health.
Other conditions influenced include rheumatoid arthritis, where shared inflammatory pathways mean gum disease can flare joint symptoms. Even cognitive health ties in, with links to Alzheimer's through neuroinflammation. The evidence is compelling: Maintaining periodontal health dampens this inflammatory fire, fostering resilience against age-related decline.
How Systemic Inflammation Manifests in Everyday Health
Systemic inflammation isn't always dramatic; it often simmers quietly, manifesting as fatigue, joint aches, or unexplained weight gain. In the context of gum disease, symptoms might start orally—red, swollen gums, bad breath, or loose teeth—but ripple outward. For heart health, this could mean increased cholesterol deposits or irregular heartbeats. Diabetics might notice erratic blood sugar readings despite consistent management.
The risks are real, but they're manageable. Authoritative bodies like the World Health Organization emphasize oral health's role in preventing non-communicable diseases. By viewing your mouth as interconnected, you empower yourself. Simple habits amplify this: Brushing twice daily with fluoride toothpaste, flossing, and using antimicrobial mouthwash reduce bacterial load, curbing inflammation at the source.
Yet, home care alone isn't enough. Professional preventive cleanings provide deep access, removing subgingival calculus that brushes miss. These appointments also include screenings for early disease detection, ensuring issues are nipped in the bud. Think of them as tune-ups for your body's inflammatory regulator.
Preventive Cleanings: Your Wellness Shield
Framing preventive cleanings as wellness essentials shifts the narrative from reactive dentistry to proactive health. These bi-annual visits aren't just about aesthetics; they're strategic interventions. During a cleaning, hygienists use tools like ultrasonic scalers to disrupt biofilms gently, followed by hand scaling for precision. Fluoride treatments and sealants add protective layers, while education on nutrition—favoring anti-inflammatory foods like leafy greens and omega-3s—ties oral care to diet.
Benefits extend beyond inflammation control:
- Enhanced Cardiovascular Protection: Regular cleanings lower C-reactive protein (CRP) levels, a marker of heart risk, as per studies in the New England Journal of Medicine.
- Better Diabetes Control: Improved gum health correlates with steadier glucose levels, reducing complication risks.
- Overall Vitality Boost: Reduced inflammation means more energy, better sleep, and stronger immunity.
In a wellness framework, these cleanings complement exercise and mindfulness. They're accessible, covered by many insurances, and yield long-term savings by averting costly treatments.
Integrating Oral Care into a Holistic Lifestyle
To make the mouth-body connection actionable, integrate periodontal care into daily routines. Start with awareness: Monitor for gum changes and consult professionals promptly. Nutrition plays a starring role—antioxidant-rich diets combat oxidative stress from inflammation.
Exercise, too, modulates immune responses, synergizing with clean oral habits. Stress management via meditation reduces cortisol, which otherwise exacerbates gum issues. Sleep hygiene ensures tissue repair, closing the loop on wellness.
For families, instill these habits early. Children with healthy gums grow into adults with lower chronic disease risks. Seniors benefit immensely, as periodontitis accelerates age-related inflammation.

Debunking Myths and Addressing Concerns
Common myths deter action: "Cleanings are painful"—modern techniques ensure comfort. "I don't have symptoms, so I'm fine"—silent progression is common. Reassuringly, most cases are reversible with early intervention.
Cost concerns? Preventive care is economical compared to treating advanced disease. Accessibility improves with teledentistry options for consultations.
The Broader Impact on Public Health
On a societal level, promoting periodontal health could ease healthcare burdens. With chronic diseases costing trillions annually, integrating oral wellness into primary care makes sense. Policy shifts, like those advocated by the CDC, underscore this.
Empowering Your Health Journey
In summary, the mouth-body connection is a powerful lever for controlling systemic inflammation. By tackling gum disease head-on, you mitigate risks to cardiovascular health, diabetes, and more. Embrace preventive cleanings as your ally in this journey—gentle, effective, and transformative.
Preventive Cleanings = Whole-Body Protection – Call Today